Leverage an Analytic Approach to Improve CMS Star Rating Performance
Improving Medicare Advantage Plan Performance through Analytics and Targeted Strategies

The CMS Star Rating program was developed to raise the quality of services provided to Medicare Advantage (MA) plan members and to empower consumers to select the highest quality plans. As the rating system continues to evolve, it is becoming increasingly difficult for providers and insurers to maintain and improve their ratings due to a variety of factors:
Retroactive guidelines are applied at the end of the year.
Annual changes to quality measures.
Annual changes to ratings cut point thresholds.
Changes in measure and category weighting factors (1x to 5x).
Plan administrators must deal with these challenges while providing great service to members and performing above average against other MA plans across 40 different quality metrics!
More specific information on the Star Ratings program can be found here:
https://www.cms.gov/stars-fact-sheet-2024.pdf
Why should plan administrators focus on Star Ratings?
Achieving an above average Star rating (4-star or above) is important for Medicare Advantage plans for many reasons. Here are a few statistics to highlight my point:
Only 42% of MA-PD contracts earned a 4-star rating (or above) in the 2024 ratings year. This is a 9% decrease from the 2023 ratings!
74% of MA-PD enrollees will select contracts with 4 or more stars in 2024.
Roughly $9 Billion in bonus payments are distributed annually to high-performing plans - an average of $417 per enrolled member.
Introducing the GLCS MA Stars Analytics Platform
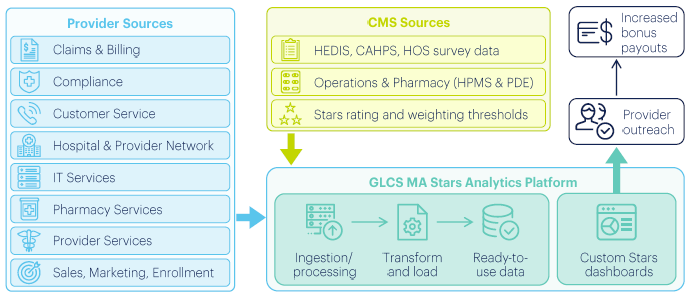
To give providers and plan administrators the insights they need to track, forecast and improve Star ratings, Great Lakes Consulting Services (GLCS) has developed an MA Stars Analytics Platform.
Core Principals
The platform was built on two core principles. First, success in Stars requires a consolidated view of quality metrics throughout each plan year. Second, a successful platform must provide plan administrators with a prospective view of ratings based on statistical and scenario modeling.
The GLCS platform is built on a dimensional data model to account for the flexibility required to track annual changes to measures, weights and cut-point thresholds. The model is informed by 10+ years of published Star rating results and paired with a set of prebuilt analytics and Tableau dashboards.
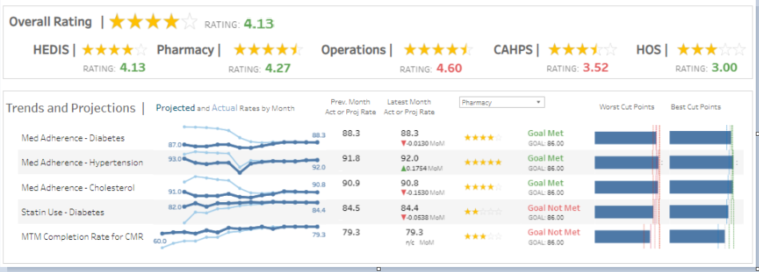
We aim to empower plan administrators, with just a few clicks, to review measure and rating projections, view historical trends by category, and spotlight areas for improvement.
The platform equips users with actionable insights needed to strategically target resources, engage clinicians, and close gaps in member care to improve health outcomes. Through data visualizations, advanced analytics and predictive modeling, we want to help plan administrators focus on the highest impact measures and take the guesswork out of year-end ratings results.
Key Analytic Categories
The GLCS platform leverages 10+ years of published rating results from CMS to predict cut-point thresholds and project ratings for each applicable quality measure. For convenience, the results are summarized from 8 Health Plan and Drug Plan categories into 5 measurement groupings and aligned to the Stars rating system:
Clinical HEDIS Member Perception
Clinical Pharmacy Improvement
Operations
To learn more about the GLCS Stars Analytics Platform, please follow the link below:
https://www.glcs.io/2023/11/GLCS_Stars_Analytics.pdf
Why GLCS?
Before our watershed partnership with JuliaHub (formerly Julia Computing) and our foray into Scientific Modeling, Simulation and Machine Learning, Great Lakes Consulting was formed from a renegade band of data wranglers. We tackled problems large and small and helped clients with data-driven solutions, including:
Enterprise Revenue Modeling
AR Valuation
Revenue Variance Analysis
Denial Analytics
Pricing Optimization
Population Health Risk Modeling
We thrive on the numerous challenges in the Healthcare space. It is always rewarding to wrestle and conform disparate data to create actionable insights and meaningful outcomes. This is still at the core of everything we do. That said, there is no bigger data challenge than MA Stars.
Looking to the Future
CMS is continuing to advance the Star ratings program. Achieving above-average Star ratings will be progressively more difficult in the upcoming years. In the measurement year 2024, CMS will:
Introduce new quality measures (Improving Physical & Mental Health).
Change the weighting factors on existing measures.
Being using online surveys for participants.
Replace Reward Factors with a Health Equity Index (HEI).
I think we are up for the challenge. We will strive to advance our platform and make every effort to help providers and plan administrators achieve and maintain high star ratings. I look forward to more blog posts to share our experiences along the way.






